This summary is based on 3 review articles about FPIES published in March 2014 in the journal Current Opinion Allergy Clinical Immunology.
What is FPIES?
Food protein-induced enterocolitis syndrome (FPIES) is a poorly understood non-IgE-mediated food hypersensitivity, primarily affecting infants and toddlers. FPIES is one of the Adverse Food Reactions (see the classification below):
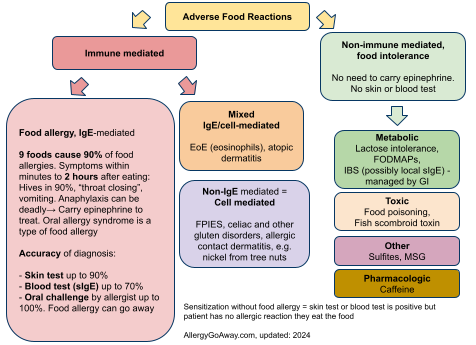
Adverse Food Reactions (click to enlarge the image).
What causes FPIES?
Foods and local intestinal imbalance between TNF-α and TGF-β play a role in the FPIES etiology.
There is regional variation in common triggering foods, rates of combined cow milk and soy FPIES and multiple food group FPIES.
WAO TV: Dr Greenhawt dfiscussed Food Protein Induced Enterocolitis Syndrome (FPIES) In a National Cohort - YouTube http://buff.ly/1jYtUS5
How common is FPIES?
PIES is regarded as a rare non-IgE-mediated gastrointestinal allergic disorder. Older nonpopulation-based studies reported an average of 1-15 cases presenting to allergy clinics a year, but recent studies have reported figures as high as 90 cases a year. The yearly incidence of FPIES in one Australian study was one in 10,000 infants less than 2 years of age. FPIES is not as rare as once thought.
What are the symptoms of FPIES?
Patients frequently present with multiple reactions, which are characterized by projectile, repetitive vomiting (emesis), dehydration, lethargy, and failure to thrive.
Chronic FPIES typically presents in neonates, whereas acute FPIES is primarily a disorder of young infants. FPIES has a slight male predominance; eczema and a family history of atopy are commonly present at diagnosis; almost one in 10 infants have coexistent IgE food allergies and siblings are rarely affected.
How to diagnose FPIES?
Despite the severity of presentation, the diagnosis is frequently delayed, and patients often undergo extensive and invasive evaluation prior to reaching the diagnosis.
How to manage FPIES?
After FPIES has been diagnosed and avoidance of the culprit food prescribed, the most important management needs are as follows:
1. Avoid recurrence of acute FPIES episodes due to accidental ingestion of culprit food. It may be useful to give patients' families an action plan.
2. The principal suggested treatments of acute FPIES episode are intravenous fluids and steroids, whereas the use of epinephrine and ondansetron requires further study. In mild-to-moderate cases, oral rehydration should be sufficient.
3. Dietary introduction of at-risk foods is a difficult area. In children with FPIES, in addition to the identified culprits, some foods may not be tolerated (typically cow's milk, legumes, cereals, poultry). It has been suggested to avoid introducing these foods during the baby's first year. Otherwise, they may be given for the first time in hospital, performing an oral food challenge.
4. Acquisition of tolerance. Children affected by cow's milk-FPIES have a good chance of acquiring tolerance by the time they reach age 18-24 months. For other culprit foods, insufficient data are available to indicate the appropriate time, so that it is suggested that an oral food challenge be performed about 1 year after the last acute episode.
Where is future FPIES research headed?
Multicenter studies are necessary to reevaluate and modify the oral food challenge criteria. Research on the pathophysiology of FPIES reactions is necessary to provide insight into the evidence-based approach to diagnosis and management of FPIES. Registries are needed to understand the phenotype, triggers, and prevalence of FPIES.
References:
Definition, etiology, and diagnosis of food protein-induced enterocolitis syndrome. Feuille E1, Nowak-Węgrzyn A. Curr Opin Allergy Clin Immunol. 2014 Mar 31. [Epub ahead of print]
http://www.ncbi.nlm.nih.gov/pubmed/24686276
Epidemiology of food protein-induced enterocolitis syndrome. Mehr S1, Frith K, Campbell DE. Curr Opin Allergy Clin Immunol. 2014 Mar 31. [Epub ahead of print]
http://www.ncbi.nlm.nih.gov/pubmed/24686277
Clinical management of food protein-induced enterocolitis syndrome. Sopo SM1, Iacono ID, Greco M, Monti G. Curr Opin Allergy Clin Immunol. 2014 Mar 31. [Epub ahead of print]
http://www.ncbi.nlm.nih.gov/pubmed/24686275
What is FPIES?
Food protein-induced enterocolitis syndrome (FPIES) is a poorly understood non-IgE-mediated food hypersensitivity, primarily affecting infants and toddlers. FPIES is one of the Adverse Food Reactions (see the classification below):
Adverse Food Reactions (click to enlarge the image).
What causes FPIES?
Foods and local intestinal imbalance between TNF-α and TGF-β play a role in the FPIES etiology.
There is regional variation in common triggering foods, rates of combined cow milk and soy FPIES and multiple food group FPIES.
WAO TV: Dr Greenhawt dfiscussed Food Protein Induced Enterocolitis Syndrome (FPIES) In a National Cohort - YouTube http://buff.ly/1jYtUS5
How common is FPIES?
PIES is regarded as a rare non-IgE-mediated gastrointestinal allergic disorder. Older nonpopulation-based studies reported an average of 1-15 cases presenting to allergy clinics a year, but recent studies have reported figures as high as 90 cases a year. The yearly incidence of FPIES in one Australian study was one in 10,000 infants less than 2 years of age. FPIES is not as rare as once thought.
What are the symptoms of FPIES?
Patients frequently present with multiple reactions, which are characterized by projectile, repetitive vomiting (emesis), dehydration, lethargy, and failure to thrive.
Chronic FPIES typically presents in neonates, whereas acute FPIES is primarily a disorder of young infants. FPIES has a slight male predominance; eczema and a family history of atopy are commonly present at diagnosis; almost one in 10 infants have coexistent IgE food allergies and siblings are rarely affected.
How to diagnose FPIES?
Despite the severity of presentation, the diagnosis is frequently delayed, and patients often undergo extensive and invasive evaluation prior to reaching the diagnosis.
How to manage FPIES?
After FPIES has been diagnosed and avoidance of the culprit food prescribed, the most important management needs are as follows:
1. Avoid recurrence of acute FPIES episodes due to accidental ingestion of culprit food. It may be useful to give patients' families an action plan.
2. The principal suggested treatments of acute FPIES episode are intravenous fluids and steroids, whereas the use of epinephrine and ondansetron requires further study. In mild-to-moderate cases, oral rehydration should be sufficient.
3. Dietary introduction of at-risk foods is a difficult area. In children with FPIES, in addition to the identified culprits, some foods may not be tolerated (typically cow's milk, legumes, cereals, poultry). It has been suggested to avoid introducing these foods during the baby's first year. Otherwise, they may be given for the first time in hospital, performing an oral food challenge.
4. Acquisition of tolerance. Children affected by cow's milk-FPIES have a good chance of acquiring tolerance by the time they reach age 18-24 months. For other culprit foods, insufficient data are available to indicate the appropriate time, so that it is suggested that an oral food challenge be performed about 1 year after the last acute episode.
Where is future FPIES research headed?
Multicenter studies are necessary to reevaluate and modify the oral food challenge criteria. Research on the pathophysiology of FPIES reactions is necessary to provide insight into the evidence-based approach to diagnosis and management of FPIES. Registries are needed to understand the phenotype, triggers, and prevalence of FPIES.
References:
Definition, etiology, and diagnosis of food protein-induced enterocolitis syndrome. Feuille E1, Nowak-Węgrzyn A. Curr Opin Allergy Clin Immunol. 2014 Mar 31. [Epub ahead of print]
http://www.ncbi.nlm.nih.gov/pubmed/24686276
Epidemiology of food protein-induced enterocolitis syndrome. Mehr S1, Frith K, Campbell DE. Curr Opin Allergy Clin Immunol. 2014 Mar 31. [Epub ahead of print]
http://www.ncbi.nlm.nih.gov/pubmed/24686277
Clinical management of food protein-induced enterocolitis syndrome. Sopo SM1, Iacono ID, Greco M, Monti G. Curr Opin Allergy Clin Immunol. 2014 Mar 31. [Epub ahead of print]
http://www.ncbi.nlm.nih.gov/pubmed/24686275