Measures of small-airway function (Scond and Sacin) may be useful in monitoring the response to asthma therapy
 The clinical relevance of increased ventilation heterogeneity, a marker of small-airways disease, in asthmatic patients is unclear. Ventilation heterogeneity is an independent determinant of airway hyperresponsiveness (AHR). It improves with bronchodilators and inhaled corticosteroids (ICSs), and worsens during exacerbations.
The clinical relevance of increased ventilation heterogeneity, a marker of small-airways disease, in asthmatic patients is unclear. Ventilation heterogeneity is an independent determinant of airway hyperresponsiveness (AHR). It improves with bronchodilators and inhaled corticosteroids (ICSs), and worsens during exacerbations.This study from Australia included 105 adult patients with asthma. The indices of ventilation heterogeneity were derived by using the multiple-breath nitrogen washout technique and included:
- ventilation heterogeneity in convection-dependent airways (Scond)
- ventilation heterogeneity in diffusion-dependent airways (Sacin)
Subjects with poorly controlled asthma had worse FEV(1), fraction of exhaled nitric oxide (FeNO), Scond, and Sacin values.
In the treatment group (n = 50) spirometric, FeNO, residual volume (RV)/total lung capacity (TLC), AHR, and Scond values significantly improved. Asthma symptom control also improved. The independent predictors of a change in asthma control were changes in Scond and Sacin values.
Improvements in ventilation heterogeneity with anti-inflammatory therapy are associated with improvements in symptoms. Sensitive measures of small-airway function such as Scond and Sacin might be useful in monitoring the response to therapy in asthmatic subjects.
Editor's note: This type of research is interesting but it has little practical implication at this point. Scond and Sacin are not available as part of the standard spirometry test of the lung function.
References:
The role of the small airways in the clinical expression of asthma in adults. Farah CS, King GG, Brown NJ, Downie SR, Kermode JA, Hardaker KM, Peters MJ, Berend N, Salome CM. J Allergy Clin Immunol. 2011 Dec 19.
Small airways in asthma silent no longer - ventilation heterogeneity in "silent zone" worse with poor asthma control http://goo.gl/XABOS
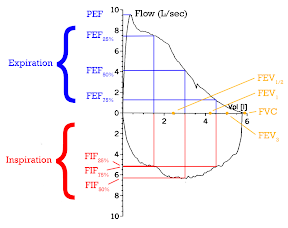
Image source: Spirometry, from Wikipedia, the free encyclopedia, GNU Free Documentation License.